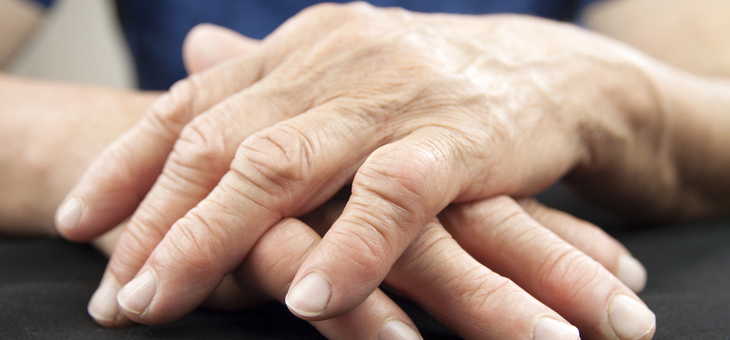
In most cases people diagnosed with rheumatoid arthritis will be able to manage the condition but it will get progressively worse as they age.
However, for about 5-10 per cent of the those diagnosed the condition can go away.
The condition affects nearly 500,000 Australians, which means that in up to 50,000 it could improve. Scientists believe they have found a way to predict those who will find improvement after their initial diagnosis, and the answer could be in your gut.
Read: Novavax to begin COVID/flu trials on older Aussies
The Mayo Clinic found that predicting a patient’s future rheumatoid arthritis prognosis could be possible by zeroing in on the trillions of bacteria, viruses and fungi that inhabit their gastrointestinal tract, known as the gut microbiome.
The findings suggest that gut microbes and a patient’s outcome of rheumatoid arthritis are connected.
Rheumatoid arthritis is the second most common form of arthritis in Australia (after osteoarthritis) and is characterised by pain and swelling in the joints, which occurs as a result of the immune system attacking the lining of the joints.
Read: COVID’s true toll revealed
The condition can eventually lead to bone and cartilage erosion, joint deformity and loss of mobility in some sufferers. Dr Jaeyun Sung, who worked on the study, said being able to predict those that would improve was a significant achievement.
Scientists have suspected for some time that the gut microbiome plays a role in rheumatoid arthritis, as well as many other inflammatory and autoimmune diseases.
“This is the first study to date that uses gut microbiome data to predict clinical improvement in rheumatoid arthritis disease activity independent of the initial measurement of their condition or prior treatment,” Dr Sung said.
The researchers analysed stool samples from 32 patients with rheumatoid arthritis at two separate clinical visits and then investigated the connection between the gut and the smallest meaningful changes in clinical disease activity and found several traits linked to future prognosis.
Read: When to see a doctor about joint pain
“By looking at patients’ baseline gut microbiome profiles, we observed significantly different microbiome traits between patients who eventually showed improvement and those who did not,” explained study co-author Dr John Davis.
By using deep-learning artificial intelligence (AI), the researchers examined if they could predict whether a patient would achieve clinical improvement and they found that they could with around 90 per cent accuracy.
This figure was high enough to showcase proof of concept that the integration of gut data and AI technology could theoretically be an avenue to predict disease course in rheumatoid arthritis patients.
“With further development, such prognostic biomarkers could identify patients who will achieve early clinical improvement with a given therapy, thereby sparing them the expense and risk of other therapies that are less likely to be effective,” Dr Davis explained.
“Conversely, such tools can detect patients whose disease symptoms are less likely to improve, and perhaps allow clinicians to target and monitor them more closely,” he said.
“Much is left to be done, but we’re on the right path toward advancing our understanding of this disease in order to individualise medicine for patients with rheumatoid arthritis.”
The researchers emphasise that every person’s microbiome is unique and consists of a complex mix of genetic, dietary and environmental influences. These differences shed light on why symptoms vary significantly among rheumatoid arthritis patients, which in turn makes it so difficult to treat and predict clinical outcome.
Do you suffer from rheumatoid arthritis? How long have you had the condition? Has it worsened over time? What do you do to limit the pain? Why not share your thoughts in the comments section below?
If you enjoy our content, don’t keep it to yourself. Share our free eNews with your friends and encourage them to sign up.