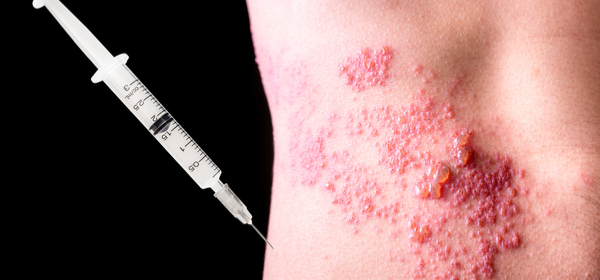
Ever had shingles? Or know someone who has?
My father developed shingles shortly after he retired. The doctor was slow to diagnose it, so he didn’t get the appropriate treatment in time to prevent serious nerve damage in one eye. His life was never the same – constant pain that peaked whenever there was a change in the weather. It was debilitating to say the least.
My sister has also had shingles. The complications nearly killed her and, again, she has to live with the complications as best she can.
Shingles is caused by the varicella zoster virus which also causes chicken pox. Once you’ve had chicken pox, the virus remains dormant in the nerve cells, controlled by the immune system. But because the immune system becomes less effective with age, the virus can be reactivated and cause shingles.
The first indication you may be getting shingles is often oversensitivity or a painful burning sensation in the affected area, usually your chest. Other symptoms can include a rash, headaches, sensitivity to light, blisters, itching and tingling.
If you develop these symptoms, you should contact your GP as quickly as possible, because early treatment can make the symptoms less severe.
This is a reminder that a vaccine is available – a single-dose injection that is recommended for all adults aged 60 years and over, unless they are allergic to any of the ingredients or have a disease that lowers their immunity.
The vaccine is free for all people aged 70 through the National Shingles Vaccination Program, with a five-year catch-up campaign in operation for anyone aged 71–79.
For those who want to be vaccinated, ask your doctor. When I got my prescription last week, I was told the cost would be about $200. Gulp, but having seen the pain it can cause, I’m saving up.
A Shingles Prevention Study of about 38,000 subjects aged 60 years and older found that the vaccine reduced the risk of shingles by 51.3 per cent and the risk of post-herpetic neuralgia (PHN), which is when the symptoms last three months or more, was reduced by 66.6 per cent.
People who have been vaccinated can still get shingles – and people who have had the disease before can get it again – but the symptoms are likely to be milder and less likely to lead to PHN.
The health department says that one dose offers protection for between five and 10 years. A booster dose is not currently recommended.
Key causes of shingles include:
- Being over 50
- A period of increased stress
- Long-term course of corticosteroids
- Any condition that affects the immune system, such as HIV/AIDS or leukaemia
- Cancer treatments such as chemotherapy or radiotherapy.
Shingles isn’t triggered by contact with someone who has chickenpox and it isn’t infectious in the same way as chickenpox. However, it can be passed on by direct contact with fluid from shingles blisters.
For more information about the shingles vaccine, speak to your GP or visit the Immunise Australia website.
Have you had shingles? Was it diagnosed in time?
Related articles:
Pain relief beyond drugs