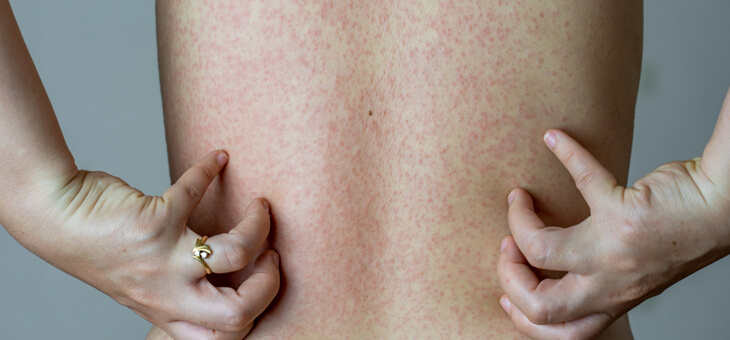
Approximately 95 per cent of Australian adults have been exposed to the chickenpox virus and are therefore at risk of developing shingles.
There are an estimated 120,000 new cases of shingles annually in Australia and the substantial burden of shingles increases over time, most prominently in the older population.
Despite how common shingles is, there’s a lot of misinformation out there. Here are seven myths and the facts to help you protect yourself.
Myth: shingles is just adult chickenpox
It’s true that shingles and chickenpox are caused by the same virus – varicella zoster – but the two are not the same.
Chickenpox occurs after initial exposure to the virus and manifests as an itchy rash that can appear anywhere on the body. The virus doesn’t disappear from the body once the rash has gone, instead, it lies dormant in the nerves.
Sometimes, the virus can be reactivated, often decades later, causing shingles that presents in a painful, blistery rash in the area of skin served by the infected nerve.
While it typically resolves in about a month for most people, it can also cause severe and long-lasting pain that is very difficult to treat.
Read: Symptoms of shingles beyond the rash
Myth: only older people get shingles
While the infection is more common in people over 50, anyone who’s had chickenpox can get shingles. Even children can get it, but the severity tends to be higher in older people.
People who are immunocompromised are also at increased risk.
Myth: you can only get shingles once
Developing shingles does not result in immunity, meaning you can still have another attack in the future. Some individuals may experience two to three episodes during their life. New attacks usually appear on different parts of the body.
Luckily, the shingles vaccine could lower your chances of a second infection, even if you get the shot after you’ve already had shingles.
Myth: the biggest problem is the rash
Though the rash is a defining sign of shingles, many sufferers report the accompanying pain to be the worst symptom.
The pain can be severe and long lasting. It typically begins a few days before the rash appears and can last a long time after – sometimes even up to a year.
The infection sits in a nerve beneath the skin’s surface and the affected area is often tender, swollen and inflamed.
Other symptoms include fever, headache, chills, upset stomach, muscle weakness, skin infection, scarring, and decrease or loss of vision or hearing.
Read: How to control nerve pain
Myth: you just have to wait it out
There is no cure for shingles, but antiviral medication may relieve the symptoms and help prevent complications. Treatment should be started within three days of the rash appearing.
Prescription and over-the-counter pain relievers, corticosteroids, and nerve block treatments may also help.
Myth: it’s not contagious
Coming into contact with someone who has shingles will not reactivate the virus in your body. But the open blisters of the rash can spread the chickenpox virus to someone who’s never had it. And that can lead to a later shingles outbreak.
Myth: shingles goes away after a few days
The rash frequently resolves within a few weeks. However, the effects on the nerve root may linger.
A phenomenon called post-herpetic neuralgia can persist. This is described as pain that persists 30 days after the rash has resolved and it can last for months or even years and be debilitating.
Fact: shingles can be worsened by stress
While stress may not directly cause or trigger shingles, there is a link between the two.
Periods of extreme stress can wear away at the body’s immune system, lowering its ability to defend against all sorts of viruses – shingles included.
Fact: it can cause vision loss
In 10 to 20 per cent of people with shingles, the rash appears in and around the eye. This can cause scarring, vision loss and other problems.
If your eye or eyelid is red, swollen or painful from shingles, seek medical help as soon as possible.
Ocular shingles could lead to glaucoma, scarring, or even blindness. Blisters on the tip of your nose can be an early warning sign.
Fact: the rash can get infected
The sores of shingles can become infected with bacteria, which can delay healing. If the pain and redness don’t improve over a couple of weeks, see your GP to ensure there’s no secondary infection.
Read: The shots you need to have as you age
Fact: vaccination can help
Since 2016, the Australian National Immunisation Program has provided shingles vaccination for all people aged 70. The shingles vaccine reduces the likelihood of shingles and of post-herpetic neuralgia. Shingles can still occur in vaccinated people, but the severity of symptoms is likely to be milder and symptoms will have a shorter duration.
Have you had shingles? Have you had the vaccine? Share why or why not in the comments section below.
Health disclaimer: This article contains general information about health issues and is not advice. For health advice, consult your medical practitioner.
If you enjoy our content, don’t keep it to yourself. Share our free eNews with your friends and encourage them to sign up.