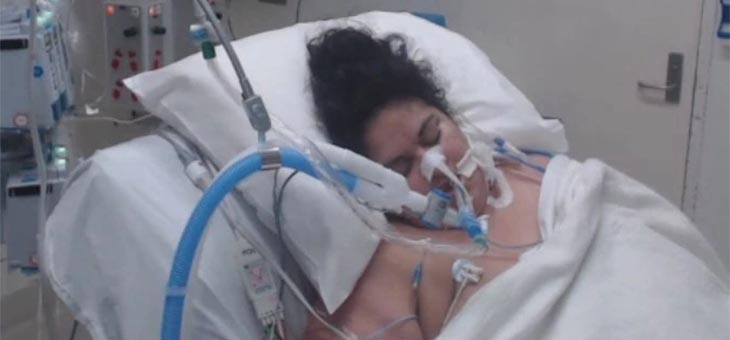
More than a year after being hospitalised with COVID-19, aged care worker Sherene Magana Cruz finds it almost impossible to talk about her experience without bursting into tears.
“I loved my job … doing activities for the residents. It could be dancing, playing games, exercise, going on bus outings, having special events and morning teas,” she said.
But now the formerly healthy 50-year-old struggles to walk unassisted.
“I was on death’s doorstep. I had no idea that COVID would lead to this at all,” she said.
“My hips are constantly in pain, which doesn’t allow me to stand for a long time and doesn’t allow me to walk for a long time.”
In July 2020, the mother of three was rushed to hospital, struggling to breathe after catching the virus from an aged care resident.
She was put into an induced coma and spent more than three weeks in an intensive care unit in Melbourne.
Physical and psychological problems
Mrs Magana Cruz is one of more than 200 ICU patients from across Australia who enrolled in a national study into the long-term effects of COVID-19 on critically ill patients.
The Monash University study, published in the international journal Critical Care today, is the first Australian study to examine the long-term impact of COVID-19 specifically in people who were in intensive care.
More than 70 per cent of respondents reported suffering persistent symptoms six months after they were hospitalised with COVID-19.
Symptoms six months after ICU:
| Symptom | Percentage of patients reporting |
|---|---|
| Shortness of breath | 34.8 per cent |
| Loss of strength | 21.7 per cent |
| Fatigue | 19.1 per cent |
| Persistent cough | 13.9 per cent |
| Loss of taste/smell | 12.2 per cent |
The most common symptom was shortness of breath, but others included fatigue, headaches, a loss of strength, and a loss of taste or smell.
A large number of participants also described impaired function and being unable to do their usual activities, said the study’s lead author, Professor Carol Hodgson, from Monash University’s School of Public Health.
“There were ongoing problems with their functioning – that could be physical function, like the ability to stand for long periods of time or walk a kilometre,” she said.
“There were problems with their psychological functioning … how they were affected emotionally by their illness or cognitive problems. So, for example, the ability to learn a new task or to focus on a task.”
People in the study were healthy before they contracted COVID-19, Prof. Hodgson said.
“These patients were reporting a very good quality of life and very minimal problems,” she said.
“There is some frustration in our survivors that they don’t understand why they’re not recovering as quickly as [they] would like to.
“Some of them may never get back to their previous level of function.”
‘Brain fog’ and shortness of breath remain
The new study adds to a growing understanding of how COVID-19 can affect the body, long after the initial infection.
In October, a clinical case definition of long COVID was announced by the World Health Organization, which they termed “Post COVID-19”.
The WHO said the condition “usually occurs three months from the onset of COVID-19 with symptoms [that] last for at least two months and cannot be explained by an alternative diagnosis”.
They say “symptoms may be new” or “persist from the initial illness” and “may also fluctuate or relapse over time”.
A recent UK study by Oxford University found one in three COVID-19 patients had long COVID three to six months after getting infected.
In Australia, more than 2300 people who contracted the virus have spent time in intensive care.
More than a year after her infection, Mrs Magana Cruz’s body is still wracked by the inflammation caused by COVID-19.
“[My] shoulders have improved a lot but the pain is still there. It restricts the strength I have to hold things,” she said.
Her ongoing symptoms include memory loss and shortness of breath, often while walking.
“Short distances are okay, but long distances, short inclines, things like that really affect the breathing,” she said.
“I forget simple words and I get stuck … I get frustrated and I really have that brain fog and sometimes I’m just sitting there in a daze thinking nothing.”
Long-term costs ‘potentially gigantic’
The new Monash University research also supports dozens of studies from around the world that show long COVID is “widespread and real”, disease researcher Professor Jeremy Nicholson from Murdoch University said.
“Once you recover from influenza, you actually pretty much completely recover. COVID is absolutely not like this,” he said.
“A lot of people think of [COVID] as just a respiratory disease, but it actually affects almost every organ in the body.”
Prof. Nicholson, who was not involved with the Monash University study, heads up the Australian National Phenome Centre (ANPC) in Perth that studies the causes and origins of disease.
Through studying thousands of blood samples from people who have had COVID-19, his team have found the virus can affect the body for months after infection.
“Very few people, even at six months, have actually metabolically, functionally recovered,” he said.
“They may have stopped coughing weeks earlier, but they’ve still got a lot of other things wrong with them.”
He said ANPC’s studies have been on people who haven’t been in hospital, yet still have long COVID.
“That’s much more worrying because millions of people have had mild symptoms from COVID, but they’re still affected,” he said.
“The long-term health economic costs of this are potentially gigantic.”
Specialised long COVID services needed
Mrs Magana Cruz said the long-term effects of COVID-19 have changed her life dramatically.
“Everything’s a lot slower … I have to learn to be patient with a lot of things,” she said.
“The good old days where you could just duck into the supermarket and get a quick present for a friend becomes a whole hour or two-hour experience.”
Specialised health services were vital to the recovery of long COVID sufferers like Mrs Magana Cruz, Prof. Hodgson said.
“At six months, if patients have ongoing physical disability or poor functioning physical function, then they need to be able to be referred to see a physiotherapist and to have ongoing rehabilitation,” she said.
“If they have poor psychological function, then they need to be referred for a psychologist and if they have poor cognitive function, then we need to address that with some sort of cognitive therapy.”
Prof. Hodgson said people with long COVID also needed more support when moving from hospital to home.
“We could perhaps manage that transition a little better, make sure that the patients are followed up, that the GPs understand how important it is to assess for physical, psychological or cognitive disabilities and refer them on to specialists for care,” she said.
Mrs Magana Cruz counts herself lucky to have had access to regular physiotherapy, massage and psychology sessions.
She hopes the ongoing specialist support she receives will help her make a full recovery.
“They’re helping me get back to that normality that I want to get back to, that physical activity that I used to do … the happy, bubbly spirit that I was.”
Her husband and children also contracted COVID while she was in hospital, but they made a full recovery.
Mrs Magana Cruz says her family and church have been her greatest support.
“I keep praying and relying on God’s strength to pull me though,” she said.
 © 2020 Australian Broadcasting Corporation. All rights reserved.
© 2020 Australian Broadcasting Corporation. All rights reserved.
ABC Content Disclaimer