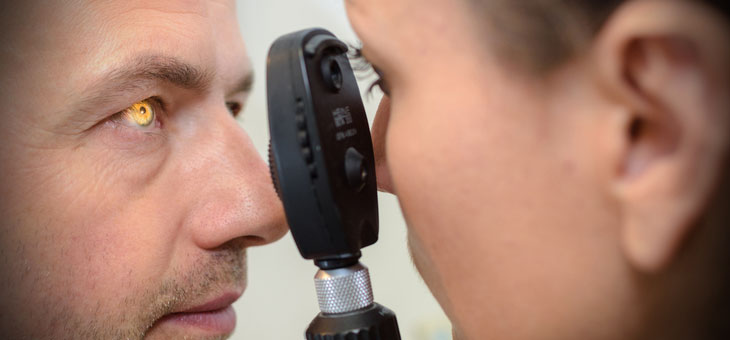
Medicine misuse is threatening the sight of 150,000 Australians, says Dr Lei Liu from Vision Eye Institute.
Glaucoma is a group of conditions that cause damage to the optic nerve which transmits signals from the eye to the brain. Damage to this nerve results in permanent vision loss or, if left untreated, total blindness.
Glaucoma affects approximately 300,000 Australians and can affect anyone. People over 40, or who have diabetes, high blood pressure, increased eye pressure and extreme short-sightedness are at higher risk. As are those with a history of steroid use, previous eye trauma or with a family history of glaucoma.
Approximately 50 per cent of people with glaucoma in Australia are undiagnosed.
There is no cure for glaucoma, but there are treatments available that slow or prevent further vision loss. Eyedrops represent the most simple and cost-effective option for managing increased pressure in the eye – the most common cause of glaucoma.
And yet, a large number of people put their sight at risk by missing or stopping doses.
“Glaucoma is called the ‘sneak thief of sight’ because it has no symptoms during the early stages,” says Dr Liu.
“Similarly, when patients skip or stop using their eye drops, they don’t usually notice any immediate effects or changes to their vision. A lot of people don’t treat eye drops like a medicine, but that’s exactly what they are.”
A study conducted on over 17,000 Australians with glaucoma revealed that 44 per cent of them stop taking their treatment within the first six months. Over half will stop after one year.
“It may seem logical to assume that if the eyes feel comfortable without treatment, then eye pressure must be within a normal range. However, this isn’t the case and further vision loss can – and does – occur without any symptoms,” says Dr Ed Boets, a consultant at Vision Eye Institute Mackay.
“Some people may experience side effects from their eye drops, such as stinging or irritation. But as with any medicine, it’s important not to discontinue treatment without consulting a healthcare professional – in this case, the prescribing ophthalmologist or optometrist.”
While some may choose to cease medication, others simply forget.
“Try to establish a routine by setting a daily alarm or administering eye drops at the same time every day, such as first thing in the morning or straight after a set meal or television program. It may also be helpful to figure out how long a bottle of eye drops usually lasts and then mark a refill date on the calendar to avoid running out,” says glaucoma specialist Dr Jason Cheng.
“Everybody responds differently to medicines, and eye drops are no different. In some people, eye drops may not reduce eye pressure as expected, or they can become less effective over time. For others, a different combination of eye drops, or perhaps glaucoma surgery – such as filtration or drainage surgery – may turn out to be a better alternative. An ophthalmologist will be able to advise the most suitable option.”
People at high risk should have regular eye tests. Everyone else should be tested every two years, even if they don’t have any concerns.
A new initiative has recently been launched to help more Australians get their eyes checked.
EyeHealth1st, a group of Australian independent optometrists, is a national early intervention campaign targeting Australians aged 40 and over, who are at higher risk of eye disease.
Glaucoma is one of the leading causes of irreversible blindness, but it’s also one of the most preventable with early detection.
“If you had to choose between your eyes and your teeth, you’d probably choose your eyes in a heartbeat,” says optometrist Jeremy Richards.
“And yet people are far more diligent about going to the dentist than they are about seeing an optometrist.”
Even those with 20:20 vision can still develop an eye disease such as glaucoma or macular degeneration. And as eyeballs age at the same time as bodies, this risk increases with age.
By 2020, more than 800,000 Australians are expected to experience vision loss or blindness. And yet, 90 per cent of vision loss and blindness is preventable with early intervention.
The national early intervention campaign for eye health hopes to reach five million Australians per month.
“This campaign is about improving the health of the eye. It’s about prevention and early detection. Most people would agree that sight is their most important sense. So we mustn’t lose sight of what’s important,” says Klaus Bartosch, managing director and co-founder of MyHealth1st.
How often do you have your eyes checked?
Related articles:
Glaucoma early warning signs
Diseases that hit with the decades
Saving your eyesight early